An interview on NPR’s Fresh Air between Terry Gross and Dr. Elisa Port, chief of breast surgery at Mount Sinai Medical Center, touched upon breast cancer screening, cancer spread, surgical removal of a healthy breast, genetic testing, and general changes in treatment over the years. Unfortunately, it missed the boat on the most hot-button issue of all. Evidence.
Published on Psychology Today, Sep. 23, 2015.
 There was an interesting interview on NPR’s Fresh Air yesterday between Terry Gross and Dr. Elisa Port, chief of breast surgery at Mount Sinai Medical Center in New York and the director of its Dubin Breast Center. Port just published a new book titled The New Generation Breast Cancer Book: How to Navigate Your Diagnosis and Treatment Options—And Remain Optimistic—In an Age of Information Overload.
There was an interesting interview on NPR’s Fresh Air yesterday between Terry Gross and Dr. Elisa Port, chief of breast surgery at Mount Sinai Medical Center in New York and the director of its Dubin Breast Center. Port just published a new book titled The New Generation Breast Cancer Book: How to Navigate Your Diagnosis and Treatment Options—And Remain Optimistic—In an Age of Information Overload.
The interview touched upon topics such as screening, cancer spreading to the other breast, surgically removing the healthy breast, the role of genetic testing, and some general changes in treatment over the years. There was no significant discussion of data or evidence to support the surgeon’s views and many of them could be called into question, but I was struck most by the mammogram conversation.
According to Dr. Elisa Port,
“This is a real hot-button issue because there are so many mixed messages that are being sent to women across this country. Mammograms are definitely the most effective way to pick up breast cancer for the general population, and that’s why the current recommendations are that every woman gets screened with a mammogram starting at age 40. Period, end of discussion.”
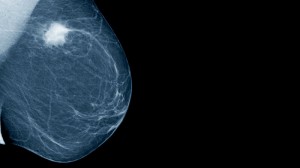
A mammogram is an X-ray picture of the breast, and there is no shortage of proponents who refer to the mammogram as “currently the most effective screening method of detecting breast cancer in its earliest, most treatable stages.” But anyone with half an ear bent toward the public debate over screening mammography in the past 15 years or so, especially a high profile journalist for a national media outlet, would know that the preponderance of evidence shows that the benefits of mammograms are much less than many of us want to believe. “Period, end of discussion” couldn’t be farther from the truth.
The problem is that some breast cancers don’t show up well on mammograms, or at all; some cancers, even though they may be small, have already spread throughout the body; and some of the most aggressive types of breast cancer show up between mammograms. In the end, “early” may not be early enough in determining prognosis. Researchers have identified at least ten molecular types of breast cancer, each associated with different prognoses. Because of cancer’s complexity, the limitations of x-rays and computer-aided technologies, as well as differences in expertise among radiologists and diagnostic centers, screening has helped to reduce the relative disease-specific death rate by only about 15 percent. Some studies put the screening-associated reduction as low as zero. And to date, very large studies have failed to find reductions in all-cause mortality for mammography screening for any age group.
The Data on Screening Mammography
Eight randomized, controlled trials of mammography screening have found that the benefits are far smaller than early evidence suggested, and the hazards have been largely ignored.
To clarify the study findings, the Harding Center for Risk Literacy prepared a facts box with neutral and easy-to-understand information about the harms and benefits of routine population-based screening. The numbers refer to 2,000 women over 50 years of age who participated in screening for 10 years (screening group), compared to 2,000 women of the same age who did not participate in the screening during the same period (control group).
 The box shows that mammography screening reduced the number of breast cancer deaths from 8 to 7 in 2,000 women. This effect had no influence on all-cancer mortality: the number of women who died of any cancer was the same in both groups. However, 200 of 2,000 women in the screening group had at least one suspicious screening result within the 10 years that later proved to be a false alarm. Since mammography screening also detects “indolent” (slowly growing or less aggressive) tumors that would never develop into life-threatening disease, their development cannot be predicted, so about 10 of 2,000 women in the screening group had their breast completely or partially removed.
The box shows that mammography screening reduced the number of breast cancer deaths from 8 to 7 in 2,000 women. This effect had no influence on all-cancer mortality: the number of women who died of any cancer was the same in both groups. However, 200 of 2,000 women in the screening group had at least one suspicious screening result within the 10 years that later proved to be a false alarm. Since mammography screening also detects “indolent” (slowly growing or less aggressive) tumors that would never develop into life-threatening disease, their development cannot be predicted, so about 10 of 2,000 women in the screening group had their breast completely or partially removed.
A 2011 analysis of the U.S. National Cancer Institute’s Surveillance Epidemiology and End Results (SEER) data found, too, that “most women with screen-detected breast cancer have not had their life saved by screening. They are either diagnosed early (with no effect on their mortality) or overdiagnosed.” In 2014, a large Canadian study with 25 years of follow-up reported that annual screening mammograms did not reduce the number of cancer deaths any more than clinical exams and health care among the nearly 90,000 women ages 40 to 59 who took part. In fact, they contributed to harm.
Recognizing the limitations of mammography screening in reducing deaths from breast cancer, the United States Preventive Services Task Force in 2009 recommended against universal mammography screens for women aged 40 to 49. The evidence revealed that when screening reduced deaths from breast cancer, it was for women between the ages 50 and 74, and screening every other year instead of annually reduced the risk of overdiagnosis. The Task Force was adamant that the decision to begin screening before age 50 is an individual one that should be made in partnership with one’s doctor. Even so, it appears that for every woman whose life is spared from a breast cancer death, another woman dies from the downstream interventions caused by screening. The group reviewed its 2009 statement again last year and made it available for public comment on April 20, 2015. The public comment period is now closed, and the Task Force is in the process of finalizing its current recommendations.
Despite the wealth of data quantifying the limited mortality benefit of screening programs (even for women ages 50 to 74) and the harms from overdiagnosis, the NPR interviewer left Dr. Port’s blanket statement about the unquestionable benefits of mammograms alone, suspended like a ton of bricks ready to crush the next unsuspecting 40-year-old whose doctor asks, “Time for a mammogram?” Instead, the conversation immediately shifted to 3-D mammograms as the next best technological advantage.
Dr. Elisa Port:
“Three-D mammography is kind of a software update to conventional imaging, where basically for a slightly higher dose of radiation it takes multiple pictures through the breast. … The way I explain it to women is it’s almost like it’s paging through a book. So rather than generating one image in one direction and a second image in the other direction you get multiple images, slices through the breast. The thing that it’s most helpful with is reducing the risk of what we call false positives.”
The analogy makes sense. Three-D imaging takes a better picture, is easier to view and catalog and, with more “slices” of the breast, might clarify those suspicious areas frequently found on 2-D mammograms, the ones that routinely encourage callbacks, retakes, and biopsies that later proved unnecessary. There is no evidence, however, that 3-D mammograms are any better at finding invasive breast cancer. If the goal is to find those potentially deadly cancers as soon as possible, then it won’t help in that regard.
And radiation is a carcinogen. That “slightly higher does of radiation” in 3-D adds up, accumulates, and carries its own inherent risk. In 2010, FDA’s Center for Devices and Radiological Health (CDRH) launched an Initiative to Reduce Unnecessary Radiation Exposure from Medical Imaging and held a public meeting on Device Improvements to Reduce Unnecessary Radiation Exposure from Medical Imaging (March 30-31, 2010). The International Commission on Radiological Protection developed two principles of radiation protection:
- Justification: The imaging procedure should be judged to do more good than harm to the individual patient. Therefore, all examinations using ionizing (high-energy) radiation should be performed only when necessary to answer a medical question, help treat a disease, or guide a procedure. The clinical indication and patient medical history should be carefully considered before referring a patient for any imaging examination.
- Dose Optimization: Medical imaging examinations should use techniques that are adjusted to administer the lowest radiation dose that yields an image quality adequate for diagnosis or intervention (i.e., radiation doses should be “As Low as Reasonably Achievable”). The technique factors used should be chosen based on the clinical indication, patient size, and anatomical area scanned, and the equipment should be properly maintained and tested.
The justification for medical radiation exposure is that the benefit outweighs the risk. Yet these guidelines urge caution because ionizing radiation penetrates below the skin, killing normal cells, mutating DNA, and generating damaging chemicals that that can lead to cancer. According to Dr. Susan Love, “The younger the breasts are, the greater the risk of radiation-causing cancer, especially if you carry the BRCA mutations” (Dr. Susan Love’s Breast Book, 6th ed., 2015, p. 155). Increased radiation exposure cannot be taken lightly.
Is it really the consensus that, “mammograms are definitely the most effective way to pick up breast cancer for the general population”?
A “period” does not end this vital discussion.
—
This article was edited since its initial publication.
—
Related:



